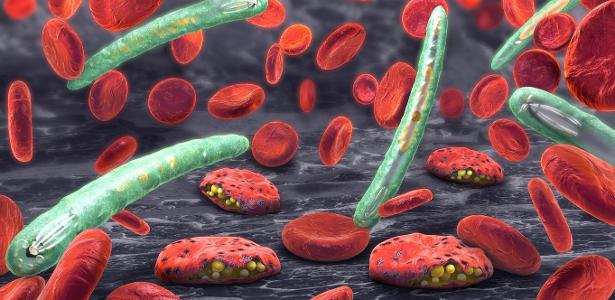
Many people fool themselves into thinking that malaria in Brazil is a problem that only worries people living in the Amazon. By the way, how warm! I say literally. Fever close to 40 degrees Celsius comes and goes every two, three or four days and this can go on for up to three years if unfortunately the sufferer does not die from the infection.
In fact, 99% of malaria cases are found there, in the north of the country. What some people forget is that people are always traveling from one place to another, and if they are visiting the area – whether for jungle tourism or for business – there is always the risk of being bitten by a mosquito one evening. anopheles, Who loves freshness at the end of the day and at night and who transmits Plasmodium, the protozoan that causes disease.
Let’s say that in other regions of the country, such as some of the Atlantic forests in São Paulo, bugs also catch them. So, in any corner of the province you can run into someone with malaria – which happens sometimes and I don’t even suspect it, which would have been a huge problem for the country’s blood banks until a few months ago.
Since September last year, however, the test known as Kit Nat Plus, developed at Bio-Manguinhos / Fiocruz. So far, he has already detected genetic material from Plasmodium in six bags donated by completely asymptomatic individuals.
It is the first test in the world capable of detecting malaria on a large scale and in an easily accessible manner in blood donated by asymptomatic people. No wonder his research has just won, to great applause, the Oswaldo Cruz Award, during International Symposium on Immunobiology Promoted by the institution itself.
More than just increasing the safety of the many people who need to receive blood components in a transfusion—cancer patients, transplant recipients, those with clotting disorders, and, in fact, a large portion of those who have surgery—the test allows SUS-related blood centers outside the North It accepts people who, out of caution, have until then been prohibited from donating blood for a long period of one year after they have traveled somewhere in the endemic area.
“The population has no idea, but if there is a lack of blood, health stops,” says biologist Patricia Alvarez. A doctor of genetics, she is responsible for the development of molecular diagnostics at Bio-Manguinhos, which developed Kit Nat Plus.
The researcher is right. With blood bank stocks always running low, it’s great to stop giving away donors, who are already so rare. Now it has become possible to find out who carries Plasmodium malaria. Therefore, the waiting period for donation after visiting an endemic area became one month.
Malaria in the first weeks
It’s in saliva Anopheles that stung someone already so infected that the plasmodium, eventually, would stop. There are more than 100 species of it around the world, but only four of them infect and cause malaria in humans.
a Plasmodium active It is by far the most common. a falciparum, a little less – fortunately, because it quickly clears all red blood cells and sometimes the creature dies without even having a chance to find out the cause. a the valley It is found only in Africa and finally malaria It tends to cause milder images.
Whatever the type, which is injected into the body through mosquito saliva, it takes no more than half an hour to reach the liver, where it multiplies in earnest, to the point that its copies explode the liver cells. It is released into the bloodstream, and begins attacking red blood cells.
By also breaking them down, it releases toxins that make the body temperature rise dramatically. There it invades more red blood cells. Then the thermometer goes down, within 48, 72 hours. Falls into circulation again, fever rises again. Even worse: It is as if the immune system has become overwhelmed, as it is able to attack the body’s own organs.
But the classic symptoms—along with fever, chills, sweat pouring in rushes, and pain that seems to blow your mind in a similar, cyclical fashion—can take a week or two to appear. In some cases, up to two months.
Antibodies, which would be a defensive response to the presence of protozoa, also take a few weeks to appear, and therefore, in this period that doctors call the immune window, it will not be useful to do a serological test to detect them. Nothing will be found.
By the way, if you have doubts, if a person really has malaria antibodies, things get complicated. Because she is not immune to a new infection, but she may not have very obvious symptoms. “It’s common in the Amazon to find people who have had malaria a few dozen times,” says Patricia Alvarez. She does not exaggerate.
Therefore, in terms of donation, blood centers had different procedures in the endemic area: there was no need to wait a year for obvious reasons, since the donor was already living there. He was ineligible to donate, of course, only if he had symptoms or knew he had malaria at that moment.

“Wannabe internet buff. Future teen idol. Hardcore zombie guru. Gamer. Avid creator. Entrepreneur. Bacon ninja.”